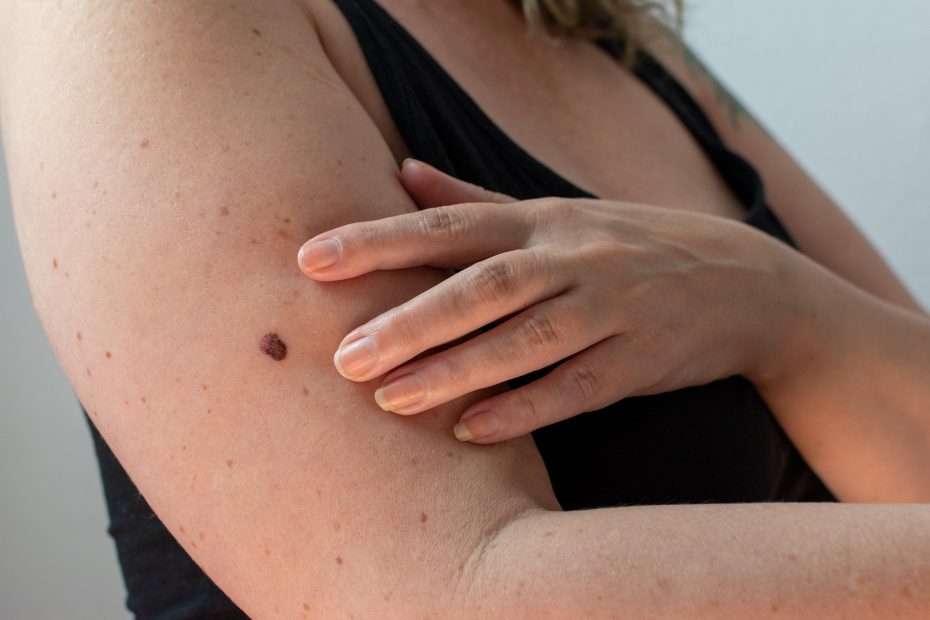
Skin Cancers are the most common type of cancers but the good news is they are amongst the easiest to spot and also have the best outcomes after treatment, in the case of non-melanoma skin cancers treated by Curaderm BEC5, there are zero recorded reoccurrences of the illness within a decade after treatment – obviously on the same part of the body.
Non-Melanoma type cancers are the most common of the skin cancers and within these the majority of cases relate to Basal Cell Carcinoma, otherwise known as BCC, which accounts for between 75%-80% of cases. The further good news is that this is the easiest of the cancers to treat, provided of course that you take action early – delay can necessitate complex reconstructive surgery or even lead to new types of cancer developing elsewhere in the body.
There is not believed to be any particular link to DNA causing this type of cancer and for this reason it is not considered to be hereditary and passed from one family member to another, e.g. parents to children. There is however a slightly puzzling correlation in that the incidence of BCC is higher if your parents have suffered from this kind of cancer previously – we suspect this is due to lifestyle similarities, for example, if your parents enjoyed holidays with long days on a hot sunny beach, it’s not only likely that you where there too, but you’ve probably also inherited the same passion and habits.
This lies at the heart of what is believed to be the main cause of non-melanoma skin cancer, it’s all about lifestyle choices. And lifestyle isn’t just the fun stuff, it also includes what you do in your working life.
The risk of getting Non-Melanoma skin cancer is highest if you have unprotected exposure to the harmful UV rays in the sun. You could be unprotected due to sunbathing without wearing an adequate sun cream for long enough or it could be because you have areas of unprotected skin, say on your face or neck. So it’s easy to imagine the risk being increased for people out and about with their job everyday delivering post, parcels, take-aways etc.
Somewhat surprisingly this risk also extends to drivers as some UV rays will penetrate vehicle windows and sunroofs. The windscreen offers better protection but other windows do not, and it’s all too easy to drive with your arm along the top of the door frame or even wind the window down and get unintentionally exposed that way. The wind chill factor of driving will of course mask some of the heat so you may not even notice you are getting burnt.
Less common these days but exposure to UV via things like sunbeds or UV lamps is also a factor and best avoided to reduce your risk of getting skin cancer. If you want a tan, apply a high quality false tan solution instead.
There are of course many healthy living factors which can help reduce your chance of getting other types of cancer and hopefully increase your chance of fighting off cancers, including skin cancer – so things like healthy eating, exercise, avoid chemicals and possible toxins, are all sensible measures to take too if you want to reduce your risks.
So, DNA does not seem to be a risk factor with regard to whether you will or won’t get Non-Melanoma skin cancer but it IS still worth taking note of what’s happened in your family as their habits and passions could influence what’s around the corner for you too.
If you do notice any changes in size, shape or colour of any moles, freckles or blemishes on your skin make sure to book in ASAP to talk to your Doctor or Health Professional for advice and if you are faced with long delays consider investigating whether Curaderm BEC5 could be a suitable treatment whilst you wait to avoid the likelihood of invasive medical procedures further down the line.
A Curaderm.net information resource you may wish to share with your own Doctor.